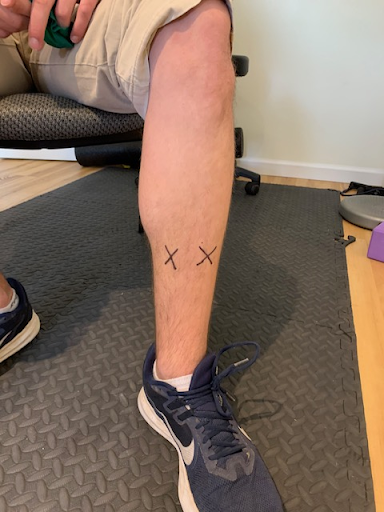
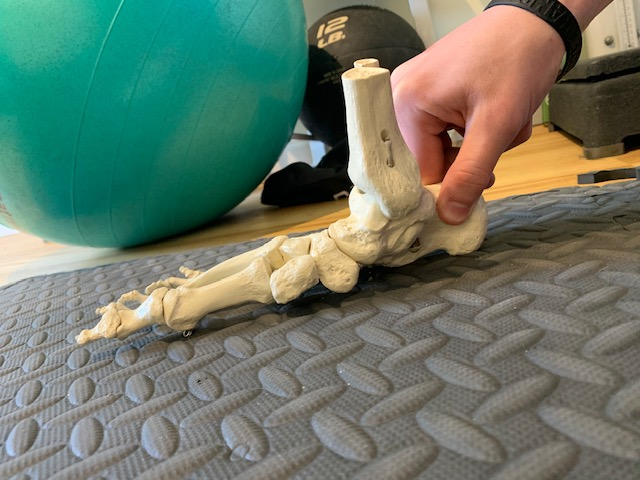
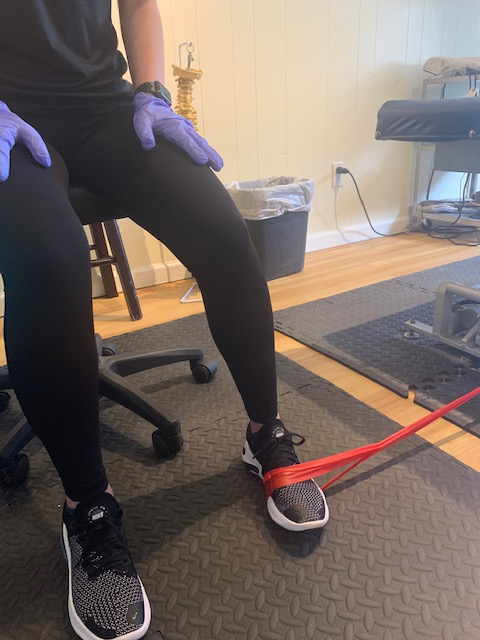
How to effectively treat “shin splints” through sports chiropractic & therapeutic exercise5/20/2020 William Brightman DC, MS, MEd If you have ever suffered from “shin splints” you know it! Shin splints is the term given to a pain along the front or back part of the tibia bone in your lower leg. It is common among runners and dancers but does not discriminate against any athlete. In fact, any athlete who has increased their intensity, duration, or frequency in training- especially running- can become afflicted with this condition. Training on hard surfaces, uneven terrain, just beginning a running program, having high arches or fallen arches, military training, and even hiking can all be contributory factors in the prevalence of shin splints. “Shin splints” is also known as medial tibial stress syndrome and the symptoms associated with this condition are tenderness, soreness, and pain that increases with the activity but can also be painful at rest. With the early onset of shin splints, rest, ice and modified activities are recommended for treatment. That is all well and good but still does not solve the problem. In fact, the problem came on with training and goes away with rest, but who says that it will not come back again when training resumes. This is when a more focused evaluation needs to be done. The sports chiropractic evaluation is a more detailed assessment that looks at all the muscles and joints in the lower extremity to look for imbalances that may be contributing to the problem. The question arises as to why some athletes are more prone to “shin splints” than others? Like most other conditions there are many reasons as to why one athlete develops shin splints while another does not. Muscular imbalances, overpronation of the foot, or even hip and pelvic distortion can contribute to “shin splints' in one athlete while the more “muscularly balanced” athlete may avoid them. This will be assessed in a sports chiropractic exam. Two specific deep muscles in the lower extremity known as the tibialis anterior and tibialis posterior muscles are found to be vulnerable in shin splints. They are deep or “core” muscles in the calf and will become weak and imbalanced with repetitive stress and lack of attention. The consequence is “shin splints”. These muscles are tested for strength during the evaluation and more often than not are weak when the athlete has shin splints. Two most common areas where “shin splints” occur (tibialis anterior and tibialis posterior muscles become strained, weak, and imbalanced→ exercise on right help to address tibialis posterior muscle Feet that overpronate and arches that fall may be a trigger to shin splints as well as other problems in the lower extremity (In addition to therapeutic exercises and adjustments, orthotics may be necessary to make correction) Measurements can be done to see how far the arch is falling and can be compared to the arch of the other foot. Discrepancies that are clinically significant may warrant sole support orthotics The athlete who trains hard and is not paying attention to good running mechanics, does not have supportive footwear, and is not strengthening the deeper core muscles of the lower extremity may become susceptible to shin splints. If muscles become weak then the corresponding joints are impacted. For instance, the tibialis posterior muscle runs down to the bottom of the foot (tarsals) and when it becomes weakened or overstretched the tarsal joints restrict and the arch overpronates. This disruption in the tarsal (foot) joints will alter the mechanics during the run and one problem becomes overpronation of the foot. This overpronation will in turn contribute to an increased stress on the posterior tibia and eventually strain the muscle where it attaches to the tibia bone. This may cause a reaction to the bone and even a possible stress response fracture. Hence the term “shin splints”. Treatment usually starts with ice and rest. Physical therapy modalities such as ultrasound and muscle stimulation may be helpful to alleviate some of the symptoms. In our practice, I have found that adjusting the tarsal bones of the feet along with performing myofascial release to the deep calf muscles is incredibly effective at restoring motion and function in the lower kinetic chain (the foot and calf region) and reducing shin splint symptoms. Secondly, the athlete needs to be on a progressive strengthening program addressing all of the muscles of the lower extremity. There should be an emphasis on the superficial and deeper calf muscles. Finally, the athlete may need a video analysis to assess their overall running mechanics. Once imbalances are pointed out exercises can be provided. This evaluative and therapeutic approach, along with lower extremity, hip, and pelvic adjustments are most effective at healing and preventing future shin splints. The sports chiropractor takes this unique approach to treating shin splints. They will combine traditional methods (ice, modalities, anti inflammatories) with biomechanical evaluation (assessing joints and muscles) and treatments (muscle and joint manipulation with corrective exercise) that are highly effective. Below are some therapeutic exercises for shin splints. This combined with extremity and pelvic adjustments, myofascial release techniques, and appropriate footwear to support overpronation (sometimes orthotics are necessary) yields the best results! Seated calf raises for soleus medial foot glide for tibialis posterior muscle Standing calf raises while squeezing ball( develops larger gastrocnemius calf muscle while hitting deeper stability muscles: performing static stretch for 15-30 seconds after exercising muscle. Squats with theraband and hip hikes to help strengthen pelvic stabilizers. ( these exercises are good for most lower extremity problems including shin splints) Active Pin & Stretch to release tibialis anterior muscle (one of the culprits in shin splints)
If you are experiencing “shin splints” consult your sports chiropractor for an evaluation and holistic approach to treatment. Several treatments combined with home instruction will correct the disorder. Diagnostic imaging (x rays, CT scan, or MRI) may be indicated if the problem has been persistent for a long period of time and has not responded to conservative treatment. Your sports chiropractor will only order these if it is absolutely necessary and the patient has not improved with care over 4-6 weeks. Standard protocol is to diagnose with examination, treat accordingly and re evaluate for progress. Results are usually superior to rest and anti-inflammatories alone. Try this multi disciplined holistic approach if you want to not only treat but prevent any future flare ups of shin splints. William Brightman DC, MS, MEd Sports Chiropractor/ Exercise Physiologist Private Practice Mahopac, NY [email protected]
0 Comments
Leave a Reply. |
AuthorDr. William Brightman has been a practicing chiropractic physician since 1998 and has been in health promotions since 1989. He currently has a successful private practice in Mahopac, NY, where he specializes in the diagnosis and treatment of joint and muscle pain. ArchivesCategories
All
|





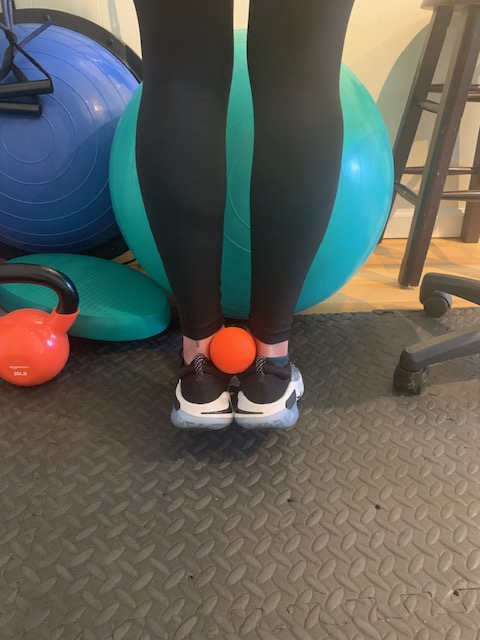



 RSS Feed
RSS Feed
